Bone Marrow Transplant Is Often The Best Treatment Available
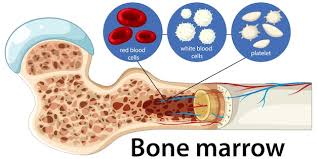
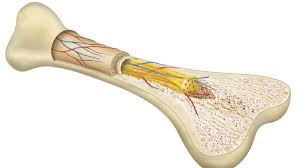
For many families, the words “bone marrow transplant” sound frightening. It is often perceived as a final, desperate step taken only when everything else has failed. In reality, Bone Marrow Transplantation (BMT)- Haematopoietic Stem cell Transplant-is not the last option; in many cases, it is the best and most definitive treatment available. To appreciate this, one must first know what bone marrow actually does. Bone marrow is the soft, spongy tissue inside our bones where life begins at a cellular level. It produces stem cells that continuously develop into red blood cells carrying oxygen, white blood cells fighting infection, and platelets preventing bleeding, and many other essential components. When this system fails, due to cancer, genetic disorders, infections, or severe immune conditions, the consequences can be life-threatening.
When the Bone Marrow Stops Working
Certain diseases directly attack or replace the bone marrow. In conditions like Acute Myeloid Leukaemia and Acute Lymphoblastic Leukaemia, abnormal white blood cells crowd out healthy cells. In Aplastic Anaemia, the marrow simply stops producing adequate blood cells. Inherited disorders such as Thalassemia and Sickle Cell Disease affect the quality and structure of red blood cells from birth. India carries a particularly heavy burden of thalassaemia, with nearly five crore beta-thalassaemia carriers and 10,000 –15,000 children born each year with thalassaemia major. For many of these children, lifelong blood transfusions become the norm. Yet, an allogeneic stem cell transplant offers something transfusions cannot, a permanent cure. In adults. Multiple Myeloma accounts for 1% of all cancers and nearly 10% of blood cancers. Here, autologous stem cell transplant significantly improves progression-free survival and remains a global standard of care. These are not “end-stage” scenarios. These are precisely the stages where timely transplant changes outcomes.
What Exactly Is a Bone Marrow Transplant?
Bone Marrow Transplantation, also known as Haematopoietic Stem Cell Transplantation, replaces damaged or diseased stem cells with healthy ones. The process is simpler than many imagine. After chemotherapy (and sometimes radiotherapy) clears diseased cells, healthy stem cells are infused through a vein, much like a blood transfusion. These cells travel to the marrow, settle there, and begin producing healthy blood cells again. This process is called engraftment and usually begins within weeks. In some cases, the patient’s own cells are used (autologous transplant). In others, stem cells come from a donor (allogeneic transplant). Siblings are ideal donors, with about a 25 % chance of being a full genetic match. Even if a matched sibling is unavailable, half-matched family donors (haploidentical) or unrelated donors from national and international registries can make a transplant possible. Today, almost every patient can find a donor.
Not Just Treatment, A New Immune System
One of the most powerful advantages of an allogeneic transplant is its ability to create a new immune system. This new immune system can recognise and destroy residual cancer cells, a phenomenon known as the graft-versus-leukaemia effect. In other words, a transplant is not just replacing cells. It is rebuilding the body’s defence system.
Understanding the Risks and the Advances
Like any major medical procedure, BMT carries risks. Temporary low immunity can lead to infections. Low platelets may increase bleeding risk. In donor transplants, graft-versus-host disease may occur. Rarely, graft failure can happen. However, modern transplant units with strict infection control, personalised monitoring, and multidisciplinary care have dramatically improved safety. Peripheral blood stem cell collection, used in about 95% of cases, is painless for donors and requires only short hospitalisation. Advances in cell processing technologies, including automated and sterile cell separation platforms, have further improved outcomes in complex and mismatched transplants. The Clinimacs cell separation machine has made transplants safer and more effective for many. But that requires a skilled operator and an experienced team.
The Message Families Need to Hear
Bone Marrow Transplant is not a “last hope” therapy. In many blood cancers and inherited blood disorders, it is the only curative option. Delaying referral can mean losing the window where transplant offers the best survival advantage. Early evaluation, proper HLA typing, and consultation with a specialised BMT team can make the difference between prolonged illness and a genuine chance at a cure. Medicine has evolved. Outcomes have improved, especially with expertise, knowledge, and technology. The availability of medicines has made a positive impact. Donor options have expanded. For the majority of patients today, Bone Marrow Transplant is not the end of the road; it is the beginning of a second life.
About the author- Dr. Joydeep Chakrabartty, Senior Consultant – Hemato Oncology and Clinical Lead – BMT Programme (Eastern Region)
